Organ Donation: Life and Death
By Lynn Frances
In September 2006, accomplished young athlete, Shane Becker, plummeted 20 feet onto cement, severely injuring his head and brain.1 Paramedics tried but could not revive him. In hospital, doctors told Shane’s mother (a nurse by profession) her son’s brain would soon be dead and there was no hope. She was approached about signing the organ donation certificate and she agreed. However, everything was on hold, waiting for Shane’s dad to arrive to say good-bye…
Like other countries, Canada requires the organ donor decision to be voluntary.
Living organ donation dates back to 1954, when a kidney from one twin was successfully transplanted into his identical brother. In 2023, many living organ donors weren’t biologically related to the recipient when they donated a kidney or part of their liver for transplantation.
Don’t lose touch with uncensored news! Join our mailing list today.
For transplantation after a declaration of “brain death” or “heart death,” an organ donation is only possible when the donor is already in a hospital near the ICU team. To remain suitable for transplantation, organs need a circulating supply of oxygen-rich blood, so the donor is put on a mechanical ventilator to support breathing.
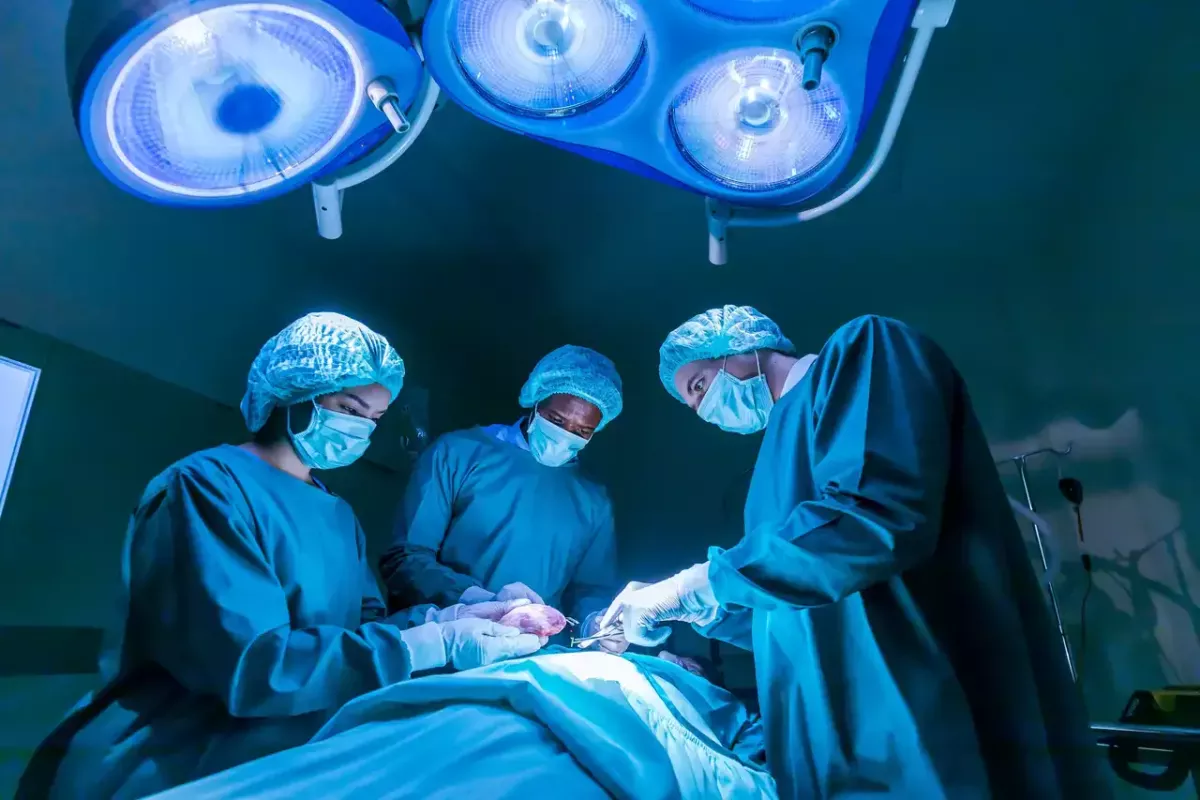
When the surgical transplant team arrives, the donor is taken to the operating room to recover the organs and tissues. Federal law states that the transplant team does not participate in the donor’s care until the determination of brain death. When an organ is recovered from the donor, it is flushed with a cooled solution to preserve it. It is packed in ice for transportation. Tissues (bone, cornea, and skin) are taken after the organs (within 24 hours).
For a heart transplant, circulation and respiration are essential to the time of excision for the organ to remain viable (four to six hours). About an hour of operating is done before the surgeon stops and removes the heart. Lungs are viable four to six hours; the liver, for up to 12 hours; kidneys, 36 hours.
Ontario Health (Trillium Gift of Life Network) is the government agency responsible for planning, promoting, coordinating and supporting organ and tissue donation and transplantation. With only 1-2% of deaths occurring near an ICU, you are six times more likely to require an organ transplant in your lifetime than to have the opportunity to be an organ donor.
Declared time of death can vary from five minutes after the heart stops (most of Canada) to 75 seconds in (Colorado), to 20 minutes (Italy). Timing is crucial if the patient is an organ donor because vital organs rapidly deteriorate when blood flow ends. The World Health Organization (WHO) is currently developing an international definition of death.
A 2005 landmark meeting of the Canadian organ transplant community set a new standard (done in the US about a decade before) for organ donation based on the “irreversible” cessation of heartbeat, called “donation after circulatory (cardiac) death” (DCD).
Under the new definition, when the patient is on the ventilator in the ICU and there is some evidence of a functioning brain, they cannot be declared “brain dead,” so “cardiac death” is used. By removing the life-supporting ventilator, they observe the patient for absence of pulse (may not be strong enough to register).
While DCD in Canada accounts for successful transplantations that otherwise would never have occurred, it has triggered intense debate in medical circles about whether the DCD donors are dead during organ “recovery.”
Shouldn’t there be extensive education about these serious matters of life and death?
Dr. Paul A. Byrne2 said that since the world’s first heart transplant in 1968, the term “cardiac death” has replaced “brain death.”
Dr. Byrne is a Board-Certified Neonatologist and Pediatrician, Clinical Professor of Pediatrics at University of Toledo, College of Medicine, and addresses this pararmount issue in his book Is “Brain Death” True Death?
“Donated organs, without exception, must come from a living person. Within minutes of ‘true death,’ the cessation of circulation and respiration, the organs will deteriorate. This is why, when organs are removed from a donor, the beating heart is always taken last. You cannot get any organs from cadavers. By then, organs are so corrupted that they are no longer suitable for transplantation. If you’re really dead, then no organs can be extracted.”
He points out differences between living and dead patients, i.e., cooling the body slows metabolism in a living person, and slows decomposition in a corpse. A ventilator, that pushes air into the lungs, only works on a living person because they can complete the oxygen and carbon dioxide exchange process. Also, if you cut the skin of someone who is living, but declared “brain dead,” the wound will heal, something that won’t happen in a cadaver.
And you would ONLY give anesthesia to someone who could still feel pain of organs being removed, not to a dead body.
Your “refusal” to be an organ donor must be documented beyond your verbal decline of “no” when renewing your driver’s license. You must “opt-out” by documenting your “refusal” in writing using “explicit language.” There is presumed consent to do all compatibility tests for organ transplantation and the treatment to keep the organs in viable condition until a matched recipient is found. Written into the consent for being an organ donor is that the organ can be used for “transplantation, education, and research.”
According to the language of US law, Revised Anatomical Gift Act (2006), “the prospective donor may have expressed the intent to have a respirator [ventilator] withdrawn in a declaration, yet it may be necessary to continue a respirator [ventilator] to assure the medical suitability of a donated part.”
Manitoba’s Final Report (2021) includes determinations, substitutions, and surprises for all provinces, some of which, like Nova Scotia, have “presumed consent” for donation of organs and tissues.
“The Commission recommends that reasonable efforts must be made to determine whether an individual consents [to] or refuses … organ and tissue donation prior to determining that deemed consent has been triggered and that donation and transplantation activities can commence. Reasonable efforts would include checking the registry for a consent or refusal, and where no consent or refusal has been registered, and where it is deemed appropriate, asking the individual or their alternate decision maker whether they wish to make a direction regarding organ and tissue donation. If after taking these steps, neither a consent nor refusal is obtained, the Commission recommends that consent should be presumed and that organ donation activities may commence.”
For Ontario Health, “When the designated facility gives notice to the Network, the Network shall determine whether the facility is required to contact the patient or the patient’s substitute concerning the right of the patient or the substitute, as the case may be, to object to the removal and use of tissue from the body of the patient for transplant.”
Canada performs more organ transplants from MAiD (Medical Assistance in Dying) donors than any country in the world.3
Choice and approval for MAiD must come first before discussing organ donation. Currently, except for Quebec and Ontario, patients initiate this conversation.
Despite concerns that the cocktail of medications used for assisted death might harm organs, studies worldwide show they are undamaged and work well after transplantation. (onlinelibrary.wiley.com/doi/10.1111/ajt.17198)
Canada is at the forefront of another emerging trend. Until recently, only those who agreed to have MAiD in hospital could donate their organs. To date, five documented cases of MAiD organ donors were given the medications at home and then, while unconscious, transported by ambulance quickly to a nearby hospital to complete the procedure and harvest the organs.
Note: A MAiD recipient can change their mind up to the final moment, so the transplant team must be ready and flexible.
…While waiting for his father to arrive and the doctors to officially declare Shane brain dead, his mother said, “We were all holding his hand, and then there was definitely some change in his grasp, especially when we spoke to him.”
Donna alerted the doctor. “His pupils that had been fixed and dilated when we initially went in were now constricted. They had changed in size. I felt sure that underneath this shell of unresponsiveness, Shane was still there, still with us, trying to tell us it was going to be okay.”
Shane remembers the frustration, “I was there cognitively; I just couldn’t show it,” trying to communicate, “Guys, I’m okay, I’m here, I’m fighting, I’m going to make it.”
If not for waiting for Shane’s dad, with the donation protocols met, their son’s organs might have been removed.
After hours of surgery, weeks in a medically-induced coma, months of rehab, and years with a damaged brain, Shane, now 32, is married and a father. “I understand that these organs are in high demand. There are long waiting lists for various types of organ donations and they save lives and, looking back on it, if I had passed away that night, I would have wanted my body to go to some good use and help people. But on the other side of the story, there’s so much of life and medical stuff, more specifically the brain, that they just don’t know about and can’t explain.”
References:
1. youtube.com/watch?v=DUn77hRK6D0 Dead Enough, The Fifth Estate
2. youtube.com/watch?v=YmjeW9Ij5ac&t=13s Dr. Paul Byrne
3. ctvnews.ca/health/canada-performing-more-organ-transplants-from-maid-donors-than-any-country-in-the-world-1.6234133